Damage caused by oxidative stress

The problem: damage caused by oxidative stress




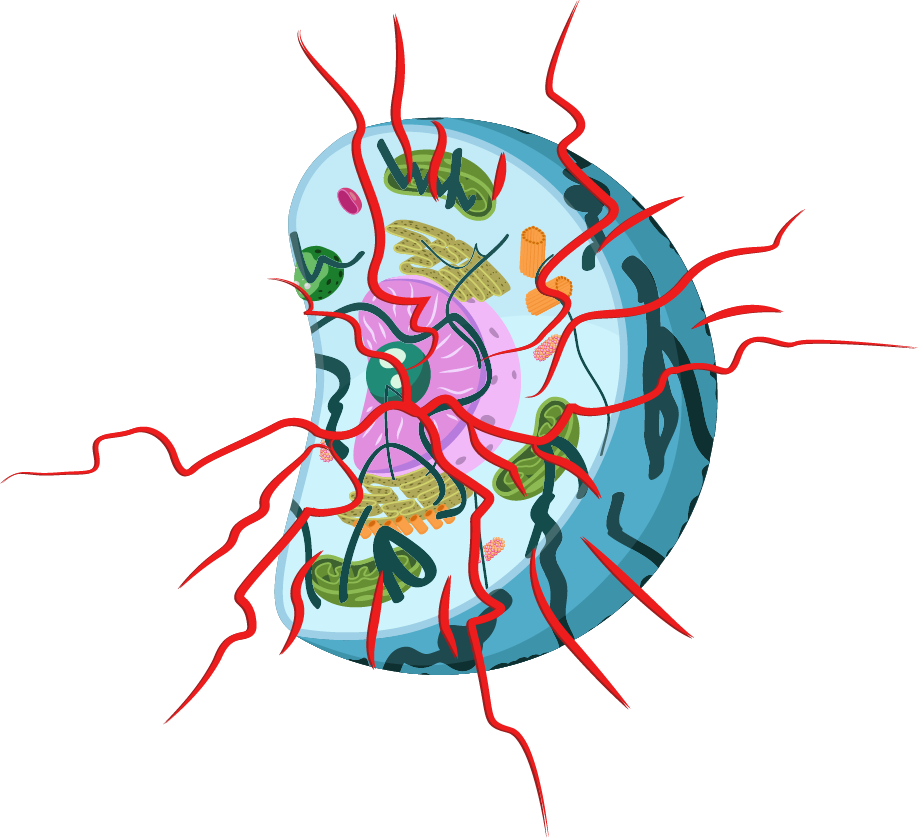
Cell damage to proteins caused by free radicals hinders:
• DNA repair
• Mitochondrial repair
• Many metabolic processes
• Countless cellular activities
All cellular activity requires energy. When a cell obtains energy from oxygen and glucose, free radicals are always produced. Some of these free radicals are in an excited, high-energy state and release this electromagnetic energy into the surrounding water. Regardless of whether they are excited or not, free radicals inevitably cause oxidative stress, damaging all cell components.
This triggers a vicious cycle: the more active a cell is, the more free radicals it produces, and the greater the damage it sustains. Proteins are particularly vulnerable. Damage from oxidative stress leads to the unfolding of their complex 3D structures. Once unfolded, proteins lose their ability to perform vital functions and cell repair. This includes repairs to DNA and mitochondria for energy production. As oxidative damage increases, cell activity decreases. Over time, this cumulative damage contributes to aging processes, diseases, and both physical and mental decline.
Effects of oxidative stress
Oxidative stress has profound effects on the human body. The cellular damage, which occurs at the molecular level (proteins, DNA, lipids), manifests in everyday life as:
- Impaired function
- Reduced performance
- Accelerated aging
- Development of chronic diseases
Here is a detailed breakdown of how these problems manifest in our lives and what causes them:
Loss of function
How it is noticeable:
- Cognitive performance: Difficulty concentrating, memory problems ("brain fog"), slower thinking. Damage to neurons and neurotransmitters by ROS impairs normal brain function.
- Muscular function: Reduced muscle strength and endurance, longer recovery times after physical exertion, muscle pain.
- Immune function: More frequent infections, as immune cells are weakened by oxidative stress and their ability to fight off pathogens diminishes.
- Sensory functions: Impairment of vision (e.g., cataracts, macular degeneration) or hearing in old age, often caused by oxidative stress in sensitive tissues.
Performance loss
Performance decline refers to the reduced efficiency of the entire organism in producing and utilizing energy.
How it manifests:
- Chronic fatigue: A persistent feeling of exhaustion that cannot be relieved by sleep. This occurs because the mitochondria (the energy producers) are damaged and can no longer provide enough ATP (cellular energy).
- Reduced energy and vitality: Lack of drive and motivation, both physical and mental.
- Reduced stress resistance: The body is less able to respond to physical or mental stress, leading to faster burnout.
- Poorer recovery: Wounds heal more slowly, and it takes longer to recover from injuries or stress.
Aging
Oxidative stress is considered one of the main causes of the cellular aging theory (the “Free Radical Theory of Aging”). It accelerates the natural aging process in both visible and invisible ways.
How it manifests:
- Skin aging: The most common and visible consequence. Reactive oxygen species (ROS) damage collagen and elastin, which give skin firmness and elasticity. This leads to wrinkles, age spots, dryness, and a dull complexion.
- Biological age vs. chronological age: People exposed to high levels of oxidative stress (e.g., through smoking, poor diet, pollution) often look older than their actual age.
- Cellular senescence: Cells stop dividing and die. The accumulation of these aged cells contributes to the loss of function in tissues and organs.
Chronic diseases
Performance decline refers to the reduced efficiency of the entire organism in producing and utilizing energy.
How it manifests:
- Chronic fatigue: A persistent feeling of exhaustion that cannot be relieved by sleep. This occurs because the mitochondria (the energy producers) are damaged and can no longer provide enough ATP (cellular energy).
- Reduced energy and vitality: Lack of drive and motivation, both physical and mental.
- Reduced stress resistance: The body is less able to respond to physical or mental stress, leading to faster burnout.
- Poorer recovery: Wounds heal more slowly, and it takes longer to recover from injuries or stress.
In summary: nonspecific symptoms such as fatigue and accelerated aging are often the first signs. If oxidative stress persists, it leads to more specific, diagnosable chronic diseases that severely impair quality of life.
Basic research
Research shows that oxidative stress damages proteins and prevents them from folding correctly, leading to impaired function, aging, and disease.
Oxidative stress is an imbalance between the production of reactive oxygen species (ROS), also known as free radicals, and the body’s ability to neutralize them with antioxidants. The excess ROS attack various cellular components, resulting in widespread damage.
Damage to proteins
Proteins are a primary target of reactive oxygen species (ROS) and play a crucial role in the functional impairment, aging, and disease processes caused by oxidative stress.
Protein damage has far-reaching consequences:
- Loss of function: Modified proteins, particularly enzymes, receptors, and signaling molecules, lose their biological activity, disrupting cellular processes and signaling pathways.
Accumulation of waste products: When the cell’s repair and degradation capacity (proteasome system) is overwhelmed, damaged proteins accumulate and contribute to cellular dysfunction.
Secondary stress: The accumulation of damaged proteins can trigger further stress on the cell’s protein quality control system.
Mechanisms and consequences
- Amino acid modification: ROS modify specific, oxidation-prone amino acids such as cysteine, methionine, lysine, arginine, and proline. These modifications alter the chemical composition and structure of proteins.
- Loss of structure (denaturation): The native folding of proteins is lost.
- Loss of function: Enzymes essential for metabolism lose their catalytic activity. Receptors can no longer receive signals, and transport proteins no longer function efficiently.
- Aggregation: Damaged proteins tend to aggregate and form insoluble deposits that cannot be efficiently degraded and accumulate in the cell.
Damage to other cell components
In addition to proteins, oxidative stress also damages lipids, DNA, and mitochondria, comprehensively jeopardizing cell integrity.
- Lipids (fats): Cell membranes and organelle membranes consist primarily of lipids. Lipid peroxidation is a chain reaction process in which reactive oxygen species (ROS) attack unsaturated fatty acids.
- Membrane damage: The integrity of the cell membrane is compromised, leading to increased permeability and ultimately cell death.
- Formation of toxic aldehydes: Lipid peroxidation produces secondary toxic products such as malondialdehyde (MDA) and 4-hydroxynonenal (4-HNE), which in turn react with proteins and DNA, causing further damage.
- DNA (deoxyribonucleic acid): Oxidative stress can directly damage both nuclear DNA (in the cell nucleus) and mitochondrial DNA.
- Base modifications: The most common type of damage is the formation of 8-oxo-2′-deoxyguanosine (8-OHdG), a biomarker for oxidative DNA damage.
- Single- and double-strand breaks: These breaks can lead to mutations that overwhelm DNA repair mechanisms and increase the risk of diseases such as cancer.
- Chromosomal aberrations: Major structural changes in chromosomes can occur.
- Mitochondria: Mitochondria, the “powerhouses of the cell,” are both the primary site and target of ROS damage.
- Impaired energy production: Damage to mitochondrial DNA and proteins (such as respiratory chain complexes) reduces the cell’s ability to produce ATP (energy).
- Increased ROS output: Damaged mitochondria produce even greater amounts of ROS, creating a vicious cycle of oxidative stress and mitochondrial dysfunction.
- Apoptosis (cell death): When the damage becomes too extensive, the mitochondria initiate programmed cell death.

